Building Resilient Health Systems
Swiss TPH works across service delivery, health workforce development, information systems, medicines, health financing, leadership and governance to build resilient health systems. Informed by the latest evidence, we design interventions at all levels of the health system to improve health outcomes, particularly for vulnerable populations. In addition, we facilitate policy dialogue and engage citizens by including them in health conversations and behavioural change strategies.
Primary Healthcare Strengthening
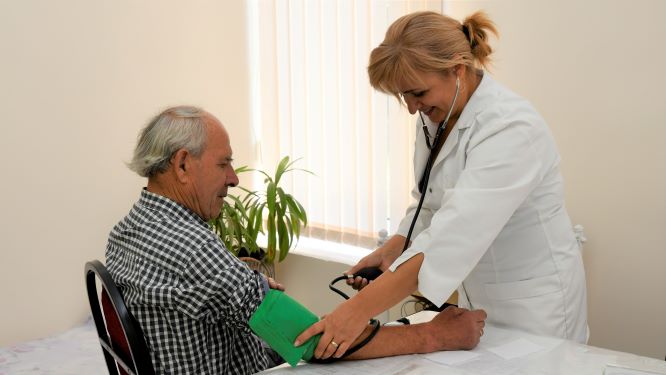
Strong primary health care (PHC) can address up to 90% of a population’s health needs by providing access to high-quality services. Health systems with resilient primary health care support with financial protection and access to care for vulnerable groups, supporting the achievement of universal health coverage (UHC) and the SDGs. Despite the promise of PHC, barriers such as cost, distance and poor quality services continue to impede access to health services. Swiss TPH works to strengthen PHC through capacity building and patient-centred quality of care as well as by engaging communities.
Family Medicine
Swiss TPH helps governments with the transformation and modernisation of health services towards decentralised, family medicine driven care and community health interventions. Health specialists at Swiss TPH work with public health institutions, service providers, local authorities and communities helping to build capacity and to put mechanisms in place to coordinate providers and share information across service interfaces towards increasing effectiveness, quality and accountability of services.
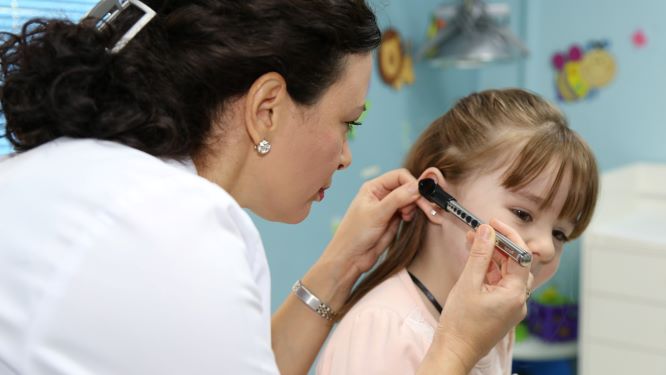
Improving the Quality of Care
Swiss TPH's main focus is to improve the quality of care in countries with insufficient health care provision. Our experts develop evidence based clinical guidelines and institutional protocols, train health personnel, develop and implement e-health based solutions and strengthen the capacity of patients and their families towards self-care.
Health Promotion
Swiss TPH has considerable experience in the design, pilot and implementation of innovative and evidence-based interventions to promote health at the level of communities, with a focus on addressing social determinants of health. We work with individuals, families, groups and communities as recommended by WHO’s IFC Framework to identify and engage vulnerable groups. Swiss TPH's approaches are based on effective community participatory techniques to identify health issues of concern, identify resources, plan responses, implement activities and evaluate results. Swiss TPH is shaping health promotion policy and promoting strategies in Tanzania, Tajikistan and Albania.
UHC and Health Financing
As passionate advocates of the drive towards UHC, Swiss TPH provides services to develop and implement health financing strategies and assess the economic viability of health system interventions. Swiss TPH undertakes situational analysis and assessment of the design, sales, servicing and sustainability of social protection mechanisms, particularly insurance schemes. Our work includes initiating and guiding policy level discussions, implementing organisational structures and developing mechanisms to include vulnerable populations.
Comprehensive Health Insurance Solutions
Swiss TPH designs and implements tailor-made health insurance solutions specifically for the informal sector and redesigns existing ones to meet contextual needs and create sustainable impact. In close collaboration with health authorities and decision-makers, we support the implementation of insurance structures and processes, operating procedures, marketing strategies, provider management and payment mechanisms, product pricing, risk pooling arrangements, and performance monitoring. An essential element of our work is to develop social health insurance mechanisms that improve the access that people have to healthcare at the time of need.
Information Management System
Swiss TPH has designed and developed an innovative Insurance Management Information System (IMIS). Through the use of mobile phones, enrollment, claims, renewal and feedback processes are optimised. The solution has proven to be cost-effective, while also being sufficiently flexible to meet different insurance needs including a centralised model in Nepal, a district-based model in Tanzania and a church-based scheme in Cameroon. Since 2017, the system forms the basis of the Swiss-German Initiative openIMIS (https://openimis.org).
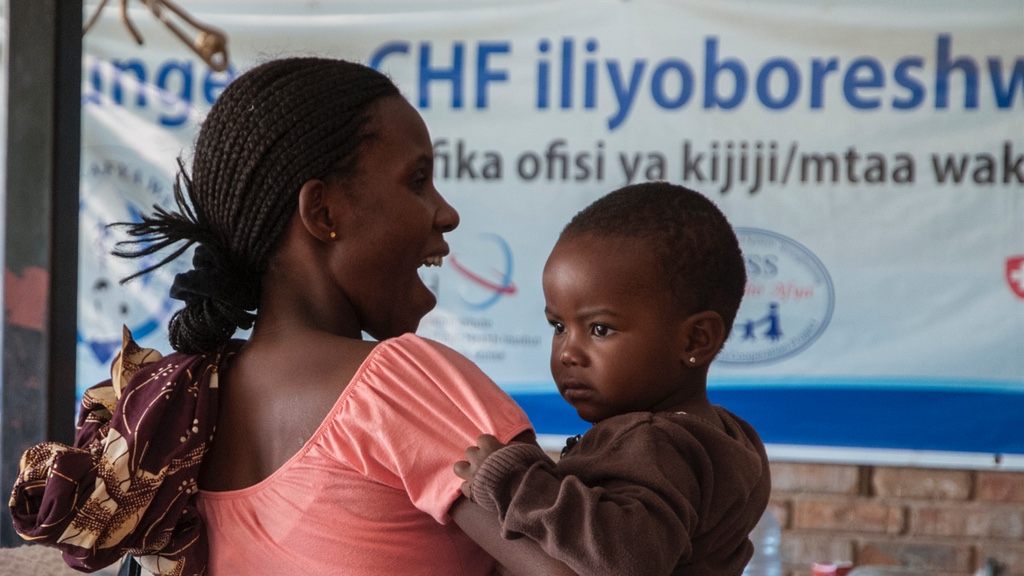
Community Health Funds
Community Health Funds function as a pre-payment mechanism for health care. Community members (especially rural households) pay an annual contribution based on a predefined household size of up to six people. These funds are matched by a government subsidy, entitling household members to access medical services and medicine without paying additional co-payments. As part of the Health Promotion and System Strengthening Project in Tanzania, funded by the Swiss Agency for Development and Cooperation (SDC), Swiss TPH works with regional and district health authorities on a comprehensive reorganisation of Community Health Funds with the aim to strengthen the health system and improve access to quality health services. The reform includs the redesign of enrollment, fund flows and reimbursement, the expansion of the benefit package and the set up of a tailor-made Insurance Management Information System (IMIS).
Health Workforce Development
Swiss TPH supports the Health Workforce 2030 Agenda with human resources planning, health worker migration and strengthening district health management. We conduct training needs assessments, develop locally adapted training courses at under- and postgraduate levels, strengthen clinical skills development and shape medical education reform. Doing so, we acknowledge required partnerships across different line-ministries involved in health workforce development, faith-based organisations and the private sector.
Our thematic portfolio (or scope) covers health staff motivation, work performance, incentive schemes and job satisfaction. Applying a gender-sensitive lens, attention is paid to health worker rights on one hand and professional and ethical codes of conduct on the other.
Medical Education Development
The Swiss Agency for Development and Cooperation’s Medical Education Development Project in Ukraine, which is implemented by Swiss TPH, works to achieve UHC through medical education. It builds on more than 10 years of experience gained in Tajikistan to reform undergraduate and postgraduate training for family doctors and nurses, and the introduction of new forms of continuous professional development, e.g. peer groups.
District Management of Health Services
In close partnership with national and local health authorities, Swiss TPH assists with the strengthening of planning, management and decision-making processes and competencies at a district level in low- and middle-income countries. This entails the building-up of functions and capacities in district management teams and their roles with regard to managing local health service delivery. This is demonstrated in several of our long-term projects in Tanzania, Ghana, Uganda, Kosovo and Moldova.
Enhancing Management
Business plans are an essential instrument to promote accountability and the autonomy of districts and their primary healthcare services. To improve management functions, Swiss TPH develops and applies tools for budget administration and execution, health information, priority planning and human resource management. Our experiences in Tajikistan, Chad and elsewhere indicate that better management also translates into improved access to healthcare services.

Striving for better governance of the health system to improve mother and child health, achieve universal health coverage and prevent epidemics through accessible healthcare.
Making an Impact

Swiss-Tajik Cooperation: Medical Education Reform
Contact

Helen Prytherch
PhD, MPH
Head of Department a.i.
+41612848686
helen.prytherch@swisstph.ch