

Basic research in infection biology
Infectious diseases are caused by pathogens - viruses, bacteria, fungi or parasites - that invade and multiply in our bodies or colonise our skin or mucosal surfaces. Pathogens infect their hosts through a variety of transmission routes, including inhalation of aerosol droplets, intimate contact with infected hosts, consumption of contaminated food, or bites from vectors such as mosquitoes or ticks.
Some pathogens invade and multiply in several or specific types of cells in our bodies, while others remain extracellular and thrive, for example, in the intestinal tract or in the bloodstream. The symptoms associated with different types of infectious diseases are equally diverse - some cause acute illness, others chronic infections, some are asymptomatic or mild, and others are severe or fatal.
Undestanding pathogen-specific biology
Regardless of the type of infectious agent, all pathogens have evolved remarkable molecular strategies that allow them to successfully infect their hosts, colonise specific parts of our bodies, tolerate or evade our immune defences, or ensure their transmission from one host to the next. Infection biologists use a variety of different experimental approaches to elucidate the functional and mechanistic basis of such pathogen- and host-specific biology and to open up new avenues for the development of new diagnostics, drugs and vaccines.
Infection biology research areas at Swiss TPH
We strive to generate new scientific knowledge in the areas of
- Virulence, survival and transmission of pathogens
- Infection dynamics and pathogenesis
- Innate and adaptive immunity
- Mechanisms and evolution of drug resistance
- Diversity, evolution and population structure of pathogens
Our researchers and students apply state-of-the-art methods in molecular biology, cell biology, biochemistry, in vitro cell culture, immunology, microbiology, genetics, population biology and bioinformatics.
Infectious diseases in focus at Swiss TPH
Our research units in the Department of Medical Parasitology and Infection Biology conduct cutting-edge basic research on infectious diseases of poverty, including
- Malaria (caused by Plasmodium spp.)
- Tuberculosis (caused by Mycobacterium tuberculosis)
- Buruli ulcer (caused by Mycobacterium ulcerans)
- Sleeping sickness/African trypanosomiasis (caused by Trypanosoma brucei).
Malaria and tuberculosis are two of the world's most devastating infectious diseases, causing hundreds of millions of clinical cases each year. Buruli ulcer and African trypanosmiasis are neglected tropical diseases that affect the poorest communities.
Malaria
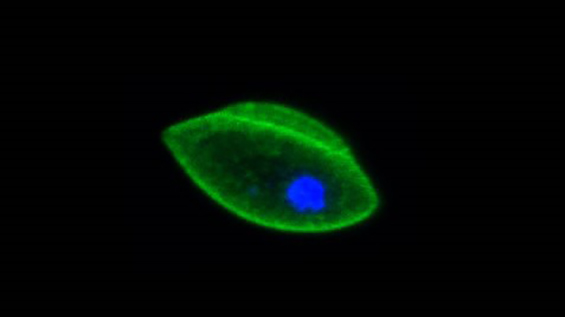
Malaria is caused by unicellular parasites of the genus Plasmodium, which are transmitted from human to human by mosquitoes. P. falciparum is accountable for the majority of severe and fatal malaria cases. P. falciparum blood-stage parasites are our main subjects of study. We are investigating several key aspects of the biology of these intracellular parasites, such as erythrocyte invasion and remodelling pathways, antigenic variation or sexual differentiation. We are also interested in understanding anti-parasite immunity in malaria pre-exposed populations and the mode of action of selected antimalarial drugs.
Sleeping sickness
Human African trypanosomiasis (also known as sleeping sickness) is caused by the flagellated unicellular parasites Trypanosoma brucei, which is transmitted by tsetse flies in several countries in sub-Saharan Africa. In humans, T. brucei multiplies extracellularly in the bloodstream and lymphatic system, known as the first stage of infection. The second stage of infection, initiated by the parasites crossing the blood-brain barrier, causes severe neurological complications and is fatal if untreated. We are investigating the molecular mechanisms of drug resistance in T. brucei using a combination of genetic and bioinformatic approaches.
Tuberculosis
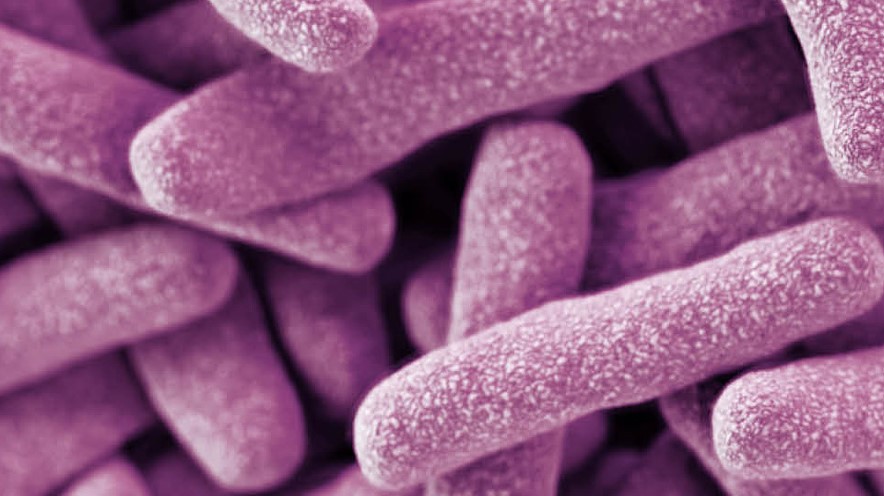
Human tuberculosis is caused by the bacterium Mycobacterium tuberculosis (Mtb). Mtb infects and multiplies most commonly in lung macrophages and spreads between people through airborne droplets, such as those released by coughing or sneezing. One of the major problems in tuberculosis control is the widespread emergence of multidrug-resistant Mtb bacteria. We combine several experimental approaches to study the evolution, distribution and ecology of Mtb drug resistance, to performt in-depth analyses of global Mtb genome diversity, and to explore aspects of the co-evolution of Mtb and human populations. We also investigate how co-morbidities, such as diabetes mellitus or helminth infections, affect tuberculosis-specific immunity.
Buruli ulcer
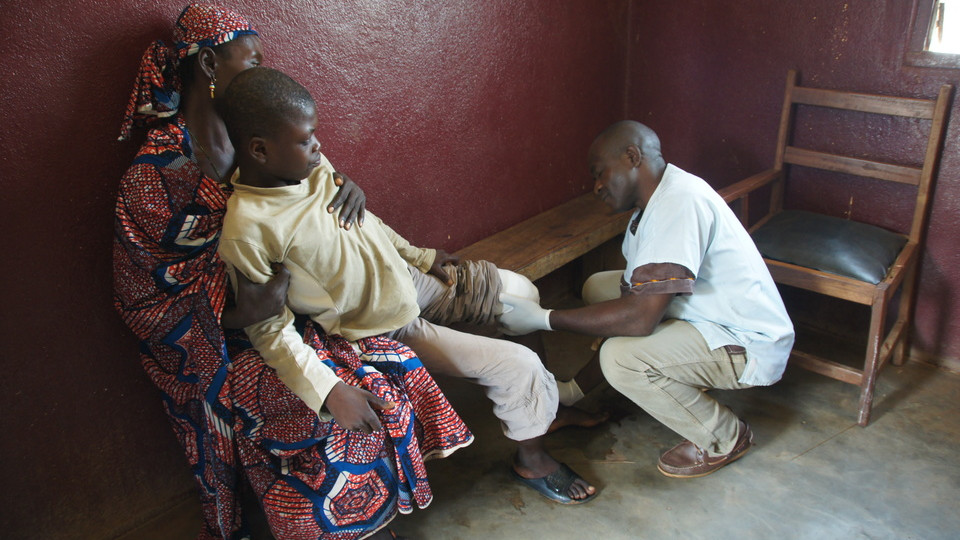
Buruli ulcer is a necrotizing skin disease that is caused by Mycobacterium ulcerans, which primarily affects people living in Western Africa. The exact mode of transmission of M. ulcerans is still unknown, but aquatic ecosystems are thought to play a central role. Unlike other mycobacterial pathogens (such as M. tuberculosis), M. ulcerans thrives mainly in the extracellular environment and causes its devastating pathology by secreting a toxin known as mycolactone. We are investigating the molecular and cellular mechanisms involved in the pathogenesis, immunology and transmission of Buruli ulcer and are seeking to unravel the pathway responsible for mycolactone-induced tissue destruction.