Clinical Tuberculosis Research
Tuberculosis (TB) remains one of the world’s leading infectious killers, disproportionately affecting people in low-resource countries, and vulnerable populations across the globe.
Our research group designs, conducts and translates high-quality clinical research to improve prevention, diagnosis and treatment of TB. We place particular emphasis on research in sub-Saharan Africa, Eastern Europe and Central Asia, where TB burden remains high and well-established partnerships ensure the development, evaluation and implementation of important innovations which are urgently needed to fight TB.
Our research focus
Prevention of TB
Preventing progression from latent TB infection to active TB is central to reducing transmission and long-term disease burden. Our research aims to improve diagnostic tools and optimising preventive treatment strategies. We focus on generating evidence to support safer, shorter and more effective preventive regimens, while addressing real-world challenges such as drug resistance among index-cases, safety and tolerability of new preventive regimens and their implementation in control programs.
Community-based active case finding
Waiting for people with active TB to seek care means that cases are often detected late, when the disease has advanced and transmission has already occurred in the household and the community. We investigate novel screening strategies to find TB cases in communities, bringing diagnosis and treatment closer to where people live and identifying infections earlier, even in asymptomatic disease stages.
New diagnostic tools
Rapid and accurate diagnosis of patients with TB, including timely detection of drug resistance, is fundamental to effective TB care and control. Delays in diagnosis and resistance detection contributes to ongoing transmission, poor treatment outcomes and creates potential for further drug-resistance amplification. A central pillar of our work is researching innovative diagnostic approaches in various clinical and programmatic settings, evaluating their performance, feasibility and impact under real-world conditions. This includes novel and precise technologies for resistance profiling to be integrated into patient care pathways, enabling faster clinical decision-making and more patient-centred, effective treatment strategies.
TB drug development and host-directed therapies
The global landscape of the TB treatment pipeline is primarily focused on introducing new active compounds and optimised treatment regimens to shorten treatment duration, improve safety and combat drug resistance more effectively. In addition, host-directed therapies are currently being developed to complement antimicrobial treatment by modulating the patient's immune response, with the aim of improving bacterial clearance, reducing inflammation-related tissue damage, preventing long-term lung damage and improving the quality of life of TB patients. Our group makes significant contributions to both the development of new TB drugs and host-directed treatment strategies.
Additional activities
Beyond conducting clinical research, our group provides scientific expertise to internal and external partners on protocol development, design and implementation of clinical trials in the field of TB. Team members serve as advisors and consultants to international research consortia and national TB programmes supporting the development of high-quality, context-appropriate studies in various settings.
Capacity strengthening and education are an important part of our work. We supervise PhD candidates and MSc students, along with building sustainable research network in partner organizations, institutions and countries.
Selected projects

AI-powered lung ultrasound for TB screening in primary care
Most TB patients in sub-Saharan Africa are treated at primary healthcare facilities that lack X-ray or molecular testing capabilities. The CAD LUS4TB project across Benin, Mali, and South Africa validates AI-assisted lung ultrasound for TB triage using mobile phone applications. Beyond TB, the technology enables multi-disease assessment including pneumonia and cardiovascular conditions – making diagnostic tools accessible where they are needed most. Read more
Host-directed therapies for drug-resistant TB
Rifampin-resistant TB carries a high risk of death, treatment failure and permanent lung damage. The EU-funded DRTB-HDT project is a phase 2 trial conducted across six countries which tests whether adding host-directed therapies – CC-11050, which reduces inflammation, or metformin, which boosts cellular antimicrobial activity – to standard treatment improves outcomes. If successful, these adjunctive therapies could increase cure rates and reduce the risk of lifelong disability in patients with drug-resistant TB. Read more
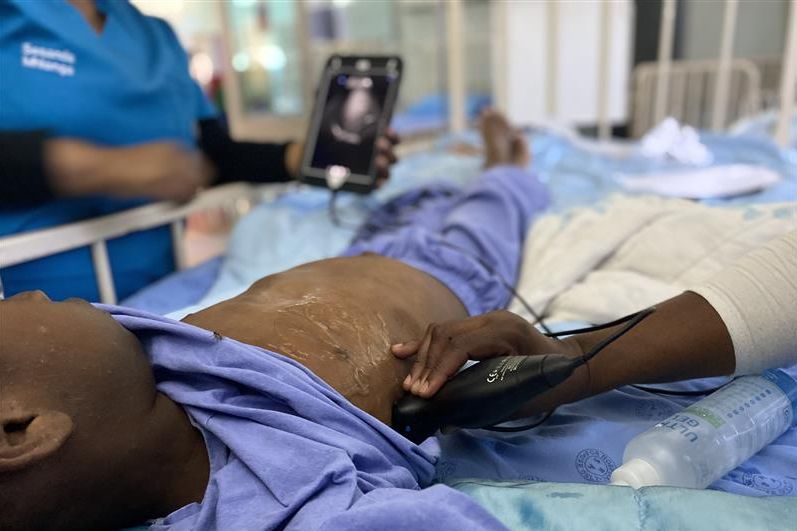
Ultrasound diagnostics for childhood pneumonia in Sub-Saharan Africa
Current pneumonia guidelines fail to distinguish severe bacterial infections from viral illnesses, resulting in inappropriate antibiotic use and missed TB cases. The Pan-African-EU partnership IMCI-PLUS is evaluating the use of point-of-care lung ultrasound in paediatric care through a trial involving 8,500 children across three countries. By developing AI-enabled tools and co-designed implementation strategies, the project aims to transform respiratory infection management. Read more

CRISPR-based point-of-care diagnostics for TB
Nearly a quarter of TB cases go undiagnosed, and drug resistance exceeds 50% in worst-affected regions. The CRSIP4TB project develops an affordable, portable diagnostic platform using laser-induced graphenization and CRISPR-Cas biosensing to detect TB and 14 resistance markers from blood samples. Swiss TPH validates the technology using biobanked samples and conducts a clinical proof-of-concept study in Georgia to estimate diagnostic accuracy in real-world settings. Read more
Subclinical TB and the virulence-transmission trade-off
Half of individuals who excrete live TB bacilli report no symptoms. This project investigates whether subclinical TB is an evolutionary strategy that allows "ancient" MTBC lineages to extend the infectious period compared to "modern" lineages. Working in Tanzania, we compare transmission dynamics, host responses, and bacterial characteristics between subclinical and active TB to understand this understudied public health phenomenon. Read more
Collaborations and networks
Clinical TB research relies on strong, sustained international partnerships. Our work is anchored in long-standing collaborations with the Ifakara Health Institute in Tanzania and the National Centre for Tuberculosis and Lung Disease in Georgia, where we jointly conduct clinical trials, diagnostic studies and capacity-strengthening activities in high-burden settings.
Beyond these core partnerships, we collaborate with academic institutions, national TB programmes and public health organisations across Central Asia, sub-Saharan Africa, Europe and the Americas. Through these partnerships and broader networks, we conduct high-quality studies, provide training and mentoring for students and young scientists, and contribute to building research capacity in TB-endemic settings. This collaborative approach ensures that research addresses real-world challenges and that knowledge gained translates into improved health outcomes where they're needed most.


 Teona Avaliani
Teona Avaliani
 Nino Maghradze
Nino Maghradze
 Klaus Reither
Klaus Reither
 Nestani Tukvadze
Nestani Tukvadze