Supporting the National Malaria Control Programme of Papua New Guinea

Swiss TPH has a long history of collaborating with partners in Papua New Guinea (PNG), a country of almost 9 million people which accounts for 80% of all malaria cases recorded in the Western Pacific Region.
Since 2004, the PNG National Malaria Control Program (NMCP) has received financial support in the form of grants from the Global Fund. The NMCP's main strategies include vector control using long-lasting insecticidal nets (LLINs) and the prompt diagnosis and treatment of malaria cases with artemisinin-based combination therapy.
In partnership with the Papua New Guinea Institute of Medical Research (PNGIMR), we support the NMCP by generating evidence of the outcomes and impact of the malaria control interventions implemented across PNG. We conduct operational research studies to identify and validate complementary approaches that could help accelerate PNG's progress towards malaria elimination.
Ongoing Projects
Evaluation of the PNG National Malaria Control Programme
Together with the PNG Institute of Medical Research, we assess the outcomes and impact of the Global Fund-supported NMCP. Major activities include national Malaria Indicator Surveys (5 MIS conducted to date), country-wide Health Facility Surveys, and analytical work to contribute to the stratification of malaria risk across PNG. Surveys provide a platform for additional studies, for example to evaluate the longevity of mosquito nets. Findings from these activities support the effective implementation of malaria control activities by the NMCP.
Highlights of Completed Projects
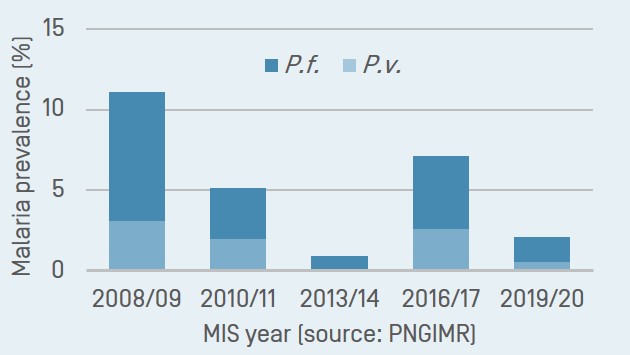
Malaria Indicator Surveys Document Changes in Malaria Prevalence
Five national Malaria Indicator Surveys (MIS) conducted since 2008 have documented a substantial decrease in the country-wide prevalence of malaria infections in the population following the scaling-up of vector control with insecticide-treated bednets. A resurgence was observed in 2016/17 and a renewed decrease in the last MIS in 2019/20. Coverage with mosquito nets has plateaued since 2011. All PNG MIS reports are available on https://www.malariasurveys.org/

School Malaria Survey in the Highlands of Papua New Guinea
In the Highlands of PNG, the climate is generally unsuitable for stable malaria transmission, providing an opportunity for complete interruption of local transmission and sub-national elimination. We conducted a school malaria survey combined with reactive case detection in Highlands communities and found only 13 malaria infections among over 6600 participants. A history of recent travel to coastal provinces was a strong predictor of infection. The findings indicate a conducive epidemiological setting for pushing towards local malaria elimination, if operational capacities allow.

Understanding Heterogeneities in Malaria in Papua New Guinea
Data from sentinel surveillance sites provide a detailed picture of trends in clinical malaria cases over time complementing national routine statistics. We used sentinel site malaria data to evaluate species-specific morbidity trends and estimate the relative impact of malaria control interventions. We found that repeated mosquito net distributions, but not the introduction of more effective treatment, reduced the incidence of clinical malaria. Human and mosquito behavior may be important drivers of ongoing malaria transmission. Link to Project
Partners and Collaborators
Documentation Centre
Malaria Indicator Survey (MIS) Reports
- Papua New Guinea Malaria Indicator Survey 2022-2023: final report on malaria prevention, infection prevalence, and treatment seeking
- Papua New Guinea Malaria Indicator Survey 2019-2020: Final Report on Malaria Prevention, Infection Prevalence, and Treatment-Seeking
- Papua New Guinea Malaria Indicator Survey 2016-2017: Malaria Prevention, Infection, and Treatment. PNGIMR, 2018
- Insecticide-treated nets and malaria prevalence, Papua New Guinea, 2008-2014
- The Papua New Guinea National Malaria Control Program: Primary Outcome and Impact Indicators, 2009-2014. PNGIMR, 2014
- Report on countrywide household survey 2010/11: Malaria control intervention coverage and prevalence of parasitaemia. PNGIMR, 2012
- Papua New Guinea/The Global Fund Round 3 Malaria Control Programme Evaluation 2008/2009: Results from Cross-Sectional Surveys and Sentinel Sites. PNGIMR, 2010
