Evolution and ecology of drug resistance
What is the Origin of Drug Resistance?
One of the most important questions in the epidemiology of drug-resistant TB is whether the global burden of drug resistance is primarily due to the de novo acquisition of resistance during patient treatment or a consequence of transmission of already drug-resistant strains.
Heterogenity in Transmission
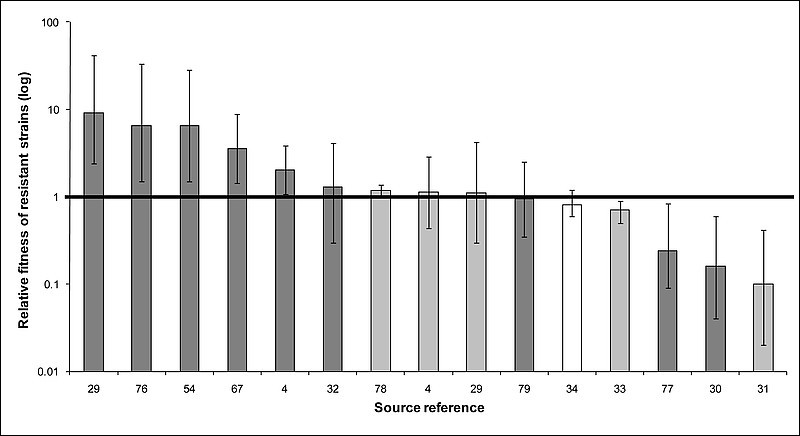
Traditionally, the thought was that drug resistance in bacteria was universally associated with a reduction in virulence and/or transmissibility. However, when reviewing the current evidence for the transmissibility of drug-resistant Mtb, we found that multidrug-resistant strains of Mtb were everything from 10 times less- to 10 times more transmissible than drug-susceptible strains (Figure 1).Compensatory Mutations
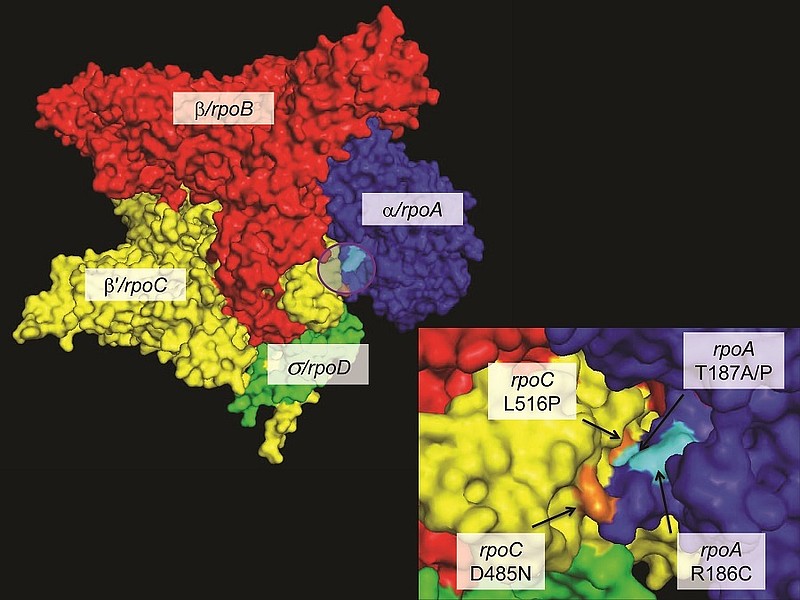
The reason for this heterogeneity is partially because the molecular basis of drug resistance in Mtb is complex, and different drug resistance-conferring mutations are associated with different effects on strain fitness. Moreover, by using a combination of experimental evolution, molecular epidemiology and comparative genome sequencing of clinical strains, we identified compensatory mutations in the RNA polymerase which mitigate some of the negative effects associated with rifampicin resistance in Mtb (Figure 2).
These compensatory mutations were associated with increased fitness in vitro and were overrepresented in regions with high burden of multidrug-resistant TB, illustrating some of the bacterial factors that could lead to the observed heterogeneity in transmission of drug-resistant Mtb.