Unit | Helminth Drug Development

We maintain a unique and extensive range of helminth life cycles for our drug discovery work. Furthermore, we are developing assays to screen promising molecules for drug discovery. Another focus of our research is preclinical work. We investigate the drug disposition and metabolic parameters of antihelminthic drugs and drug development candidates. Finally, we conduct human clinical trials in endemic countries to assess the safety and efficacy of oral antihelminthic drugs or drug combinations.
Our research team is interested in identifying and developing novel, broad-spectrum and orally active drugs against helminth diseases, including soil-transmitted helminthiasis, schistosomiasis and food-borne trematodiases.
Need for Novel Anthelminthics
Soil-transmitted helminthiasis, schistosomiasis and food-borne trematodiases affect hundreds of millions of people, particularly those living poor rural communities in low- and middle-income countries. A vaccine is not yet available and is unlikely to be any time soon. As a result, the only way to control morbidity is to administer therapeutic drugs on a regular basis. Since very few of these drugs are currently available, the development of new, safe and efficacious anthelminthics is indispensable.
Our Research Activities
The research in our unit covers a wide range of activities, from drug discovery to development, from bench work to field clinical trials. We are a multidisciplinary team of technicians, PhD students, post-doctoral fellows or civil servants trained as biologists, pharmacists, epidemiologists or medical doctors.

Jennifer Keiser
Associate Professor, PhD
Head of Unit
+41612848218
jennifer.keiser@swisstph.ch
Highlights

Clinical Development of Emodepside against Soil-Transmitted Helminthiasis
Soil-transmitted helminth infections are caused by different species of parasitic worms, including whipworms, hookworms and roundworms. Worldwide, more than 1.5 billion people are infected with at least one soil-transmitted helminth, with most of the infected population living in sub-Saharan Africa. Safe drugs are available to treat soil-transmitted helminth infections, but the efficacy varies widely. The current treatments recommended by WHO are albendazole and mebendazole. However, in the case of the whipworm Trichuris trichiura, a single dose of these drugs can cure only a handful of infected people. And with drug resistance on the rise, new alternative treatments are urgently needed. Emodepside is an anthelmintic treatment used to date in veterinary medicine. To fill the anthelmintic drug pipeline, Swiss TPH researchers have tested emodepside for the first time in humans infected with soil-transmitted helminths in Phase II trials (see publications in New England Journal of Medicine 2023 and The Lancet 2024). Swiss TPH is working with life sciences company Bayer to develop the drug further, with Phase III trials due to start in 2025. We are also conducting laboratory studies to assess drug combinations with emodepside.

Microbiome Studies
Pharmacomicrobiomic interactions between the human gut microbiota and non-antibiotic drugs have attracted significant research interest due to their proven potential to disrupt treatment outcomes. Despite this, there is a substantial knowledge gap regarding pharmacomicrobiomic interactions of anthelmintic drugs. Our group recently demonstrated a strong association between gut microbiota composition and anthelmintic efficacy against Trichuris trichiura (Nature Communications, 2022). In addition, we described the antibiotic properties of critical anthelmintic drugs against a wide range of bacterial species and their potential to induce cross-resistance to other antibiotics following anthelmintic exposure (Communications Biology, 2024). Our current research is systematically investigating these interactions to understand their contribution to treatment failure and their impact on gut microbial taxonomic and functional diversity. By gaining mechanistic insights into these interactions, we aim to unravel their role in shaping treatment outcomes and improve therapeutic strategies.
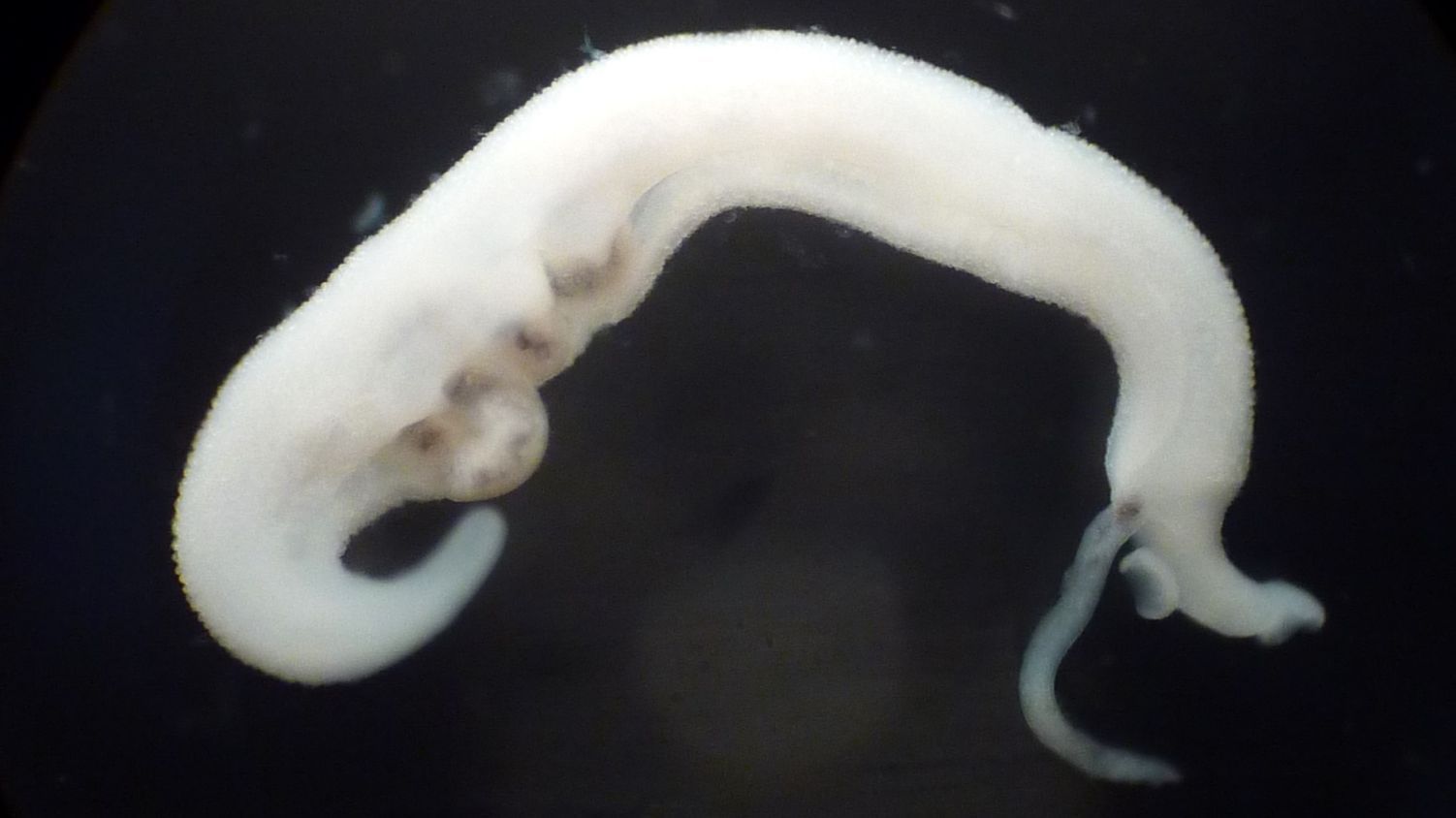
Antimalarials for Schistosomiasis
Schistosomiasis, caused by Schistosoma mansoni, S. haematobium and S. japonicum, continues to affect the health and quality of life of millions of people worldwide. Yet, we still rely on praziquantel as the sole treatment. Drug repurposing (or repositioning) is the development of new indications from existing, failed or abandoned drugs. Particular attention has been paid to antimalarials, as Plasmodium and Schistosoma spp. both utilise hemin as a common food source. The aim of this project is to investigate the antischistosomal properties of the artemisinins in vitro and in vivo, including pharmacokinetic studies. Read more

Novel Tools and Strategies for Breaking Schistosomiasis Transmission
Challenges occur on “the last mile” towards schistosomiasis elimination, including the persistence of transmission hotspots, recrudescence of infection in areas where the prevalence has been successfully reduced, and diagnostics that are not sensitive and specific enough to detect light intensity infections. In the SchistoBreak study, we explore the application of new point-of care diagnostic tools and adaptive intervention strategies that are tailored to the micro-epidemiology of schistosomiasis in the North of Pemba island, Zanzibar, United Republic of Tanzania. Read more
Collaborators
Selected Projects
All ProjectsLatest Publications
All PublicationsAjayi D.T et al. Pharmacometric analysis to describe pharmacokinetics and exposure-efficacy response of ivermectin in adolescents infected with Trichuris trichiura. J Clin Pharmacol. 2025;65(4):433-440. DOI: 10.1002/jcph.6158
Dupouy B et al. Synthesis of 1,2,3-triazole-methyl-menadione derivatives: evaluation of electrochemical and antiparasitic properties against two blood-dwelling parasites. ChemMedChem. 2025;20(6):e202400731. DOI: 10.1002/cmdc.202400731
Dziwornu G.A, Attram H.D, Häberli C, Masike K, Njoroge M, Keiser J. Benzimidazole analogues active against adult Schistosoma mansoni: SAR analyses, in vivo efficacy in mice, and preliminary mechanistic studies as potential inhibitors of hemozoin formation. Eur J Med Chem. 2025;284:117186. DOI: 10.1016/j.ejmech.2024.117186
Lo N.C et al. Review of the WHO guideline on preventive chemotherapy for public health control of strongyloidiasis. Lancet Infect Dis. 2025;25(3):e146-e152. DOI: 10.1016/s1473-3099(24)00595-4
Lotz C.N, Mrimi E.C, Schneeberger P.H.H, Ali S.M, Hattendorf J, Keiser J. Performance of real-time polymerase chain reaction and Kato-Katz for diagnosing soil-transmitted helminth infections and evaluating treatment efficacy of emodepside in randomized controlled trials. PLoS Negl Trop Dis. 2025;19(2):e0012872. DOI: 10.1371/journal.pntd.0012872

 Stefan Biendl
Stefan Biendl
 Naomi Chi Ndum
Naomi Chi Ndum
 Maude Dagenais
Maude Dagenais
 Jennifer Giovanoli
Jennifer Giovanoli
 Cécile Häberli
Cécile Häberli
 Eveline Hürlimann
Eveline Hürlimann
 Hannah Jeanguenat
Hannah Jeanguenat
 Jennifer Keiser
Jennifer Keiser
 Ursula Panzner
Ursula Panzner
 Pierre Schneeberger
Pierre Schneeberger