Epidemiology and Intervention Sciences
Our research group generates robust, field-based evidence to support the implementation of effective health programmes, with a strong focus on malaria and other infectious diseases. Our research uses a broad range of quantitative, qualitative, and mixed-methods approaches to develop and evaluate vector control, case management, and surveillance-response strategies, drawing on expertise in molecular epidemiology, modelling, population genetics, and health systems research through close collaboration with other groups.
We conduct field-based research in partnership with institutions in disease-endemic countries to assess how interventions perform under routine conditions, generating essential evidence to ensure programmes are feasible, scalable, and make optimal use of limited resources. This work is embedded within long-term research and implementation partnerships with national malaria control programmes in settings such as Tanzania, Zanzibar, and Papua New Guinea.
Through strong collaboration across Swiss TPH and with external partners, our work directly informs programmatic decision-making and health policy at national and global levels.
Our research focus
Disease epidemiology and transmission dynamics
We study the occurrence and transmission determinants of malaria and other communicable diseases with epidemiological field studies, supported by mathematical and geospatial models and molecular approaches including population genetics.
Effectiveness and impact in real-world settings
We evaluate preventive and curative interventions in routine and national programme settings, using observational and intervention studies and implementation research to understand how and why interventions work in practice.
Vector control
We evaluate the effect of vector control tools, such as insecticide-treated nets or larval source management, against malaria and other vector borne diseases in different real-world settings.
Surveillance, response and disease monitoring
We develop and assess surveillance-and-response systems that support timely case detection and targeting of interventions, including in low-incidence and elimination contexts.
Health systems and quality of care
We investigate how health system factors such as access to care, service delivery, referral pathways and quality of care shape health outcomes for patients and populations, helping to ensure that promising interventions translate into meaningful impact in real-world settings.
Selected projects

Malaria elimination in Tanzania and Zanzibar
Through the TEMT and MEZA initiatives, Swiss TPH maintains long-term collaborations with Tanzania's National Malaria Control Programme and the Zanzibar Malaria Elimination Programme. Our work supports evidence-based, cost-effective malaria control strategies at national and decentralized levels – building on the established success of previous control efforts including the NETCELL project.

Rectal artesunate for severe malaria
CARAMAL, a multi-country observational study, assessed the real-world effectiveness of pre-referral rectal artesunate for severe childhood malaria in remote settings. The research identified critical health system constraints affecting treatment outcomes, providing evidence to strengthen emergency malaria care delivery in hard-to-reach populations where timely intervention is essential. Read more

Tailored malaria control in Papua New Guinea
This long-term collaboration generates evidence to guide Papua New Guinea's national malaria strategies, including sub-national tailoring of interventions and reactive case detection approaches. Our research supports the country's transition from control to elimination by adapting strategies to local transmission heterogeneity and strengthening surveillance-response systems. Read more

Non-mesh insecticidal nets for malaria control in hard-to-reach populations
The NOMHAD study assesses the effectiveness of PermaNet® Dumuria, a mosquito net designed for mobile populations, in protecting children in nomadic and displaced communities in South Sudan and Tanzania. This operational research addresses a critical evidence gap, informing WHO guidance and humanitarian malaria policy and programme decisions for highly mobile, underserved populations. Read more
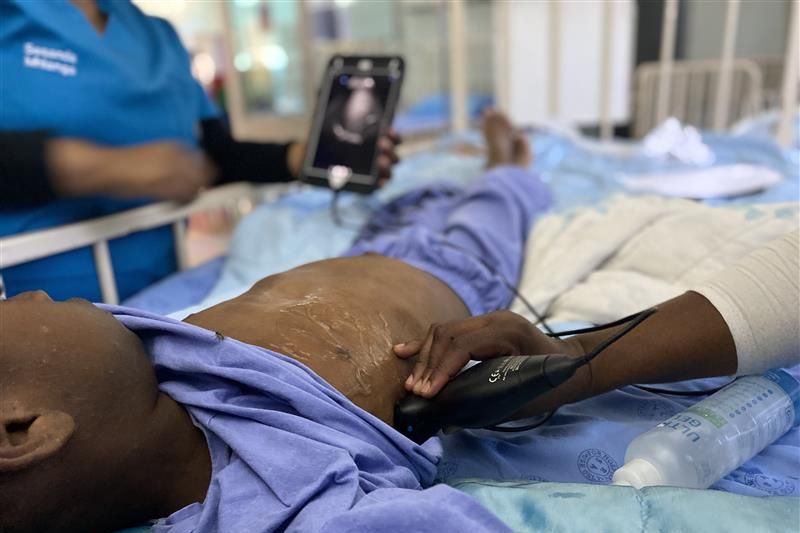
Ultrasound diagnostics for childhood pneumonia in Sub-Saharan Africa
IMCI-PLUS, an inter-disciplinary Pan-African-EU research consortium, evaluates the integration of point-of-care lung ultrasound (PLUS) into clinical management of paediatric lower respiratory tract infections – the leading cause of child morbidity and mortality in Sub-Saharan Africa. The project addresses diagnostic challenges and implementation pathways for resource-limited healthcare settings. Read more

Coordinating global malaria policy and implementation
Through GlobMal, Swiss TPH strengthens the RBM Partnership to End Malaria by coordinating three key working groups: Vector Control, Case Management, and Multi-Sectoral Action. We facilitate the global policy dialogue that shapes how countries implement malaria interventions and accelerate progress toward elimination. Read more
Collaborations and networks
The group hosts the WHO Collaborating Centre for Modelling, Monitoring and Training for Disease Control and Elimination, reflecting its contribution to the development of global technical guidance and capacity building in the field of malaria.
Our work is built on long-term partnerships with academic institutions, national health authorities, and international organisations particularly in Africa, the South Pacific, and the Europe. Key partners include institutions such as the Ifakara Health Institute and the Papua New Guinea Institute of Medical Research, alongside collaborations with national disease control programs.
The group also engages actively in global policy networks, including supporting the RBM Partnership to End Malaria through the coordination of three Technical Working Groups, ensuring that research evidence contributes to international dialogue, guidance, and collective learning.


 Duha Abuobaida Abdalla Mahgoub
Duha Abuobaida Abdalla Mahgoub
 Bakar Fakih
Bakar Fakih
 Manuel Hetzel
Manuel Hetzel
 Noela Kisoka
Noela Kisoka
 Christian Lengeler
Christian Lengeler
 Vincent Minconetti
Vincent Minconetti
 Sharon Mukankaka
Sharon Mukankaka
 Sung Hea Park
Sung Hea Park
 Gabriel Ponce de Leon
Gabriel Ponce de Leon
 Natacha Protopopoff
Natacha Protopopoff
 Osama Seidahmed
Osama Seidahmed
 Aita Signorell
Aita Signorell
 Johanna Stenstrom
Johanna Stenstrom
 Diana Timbi
Diana Timbi